Find out if you could benefit from the latest technology behind outpatient laser spine surgery.
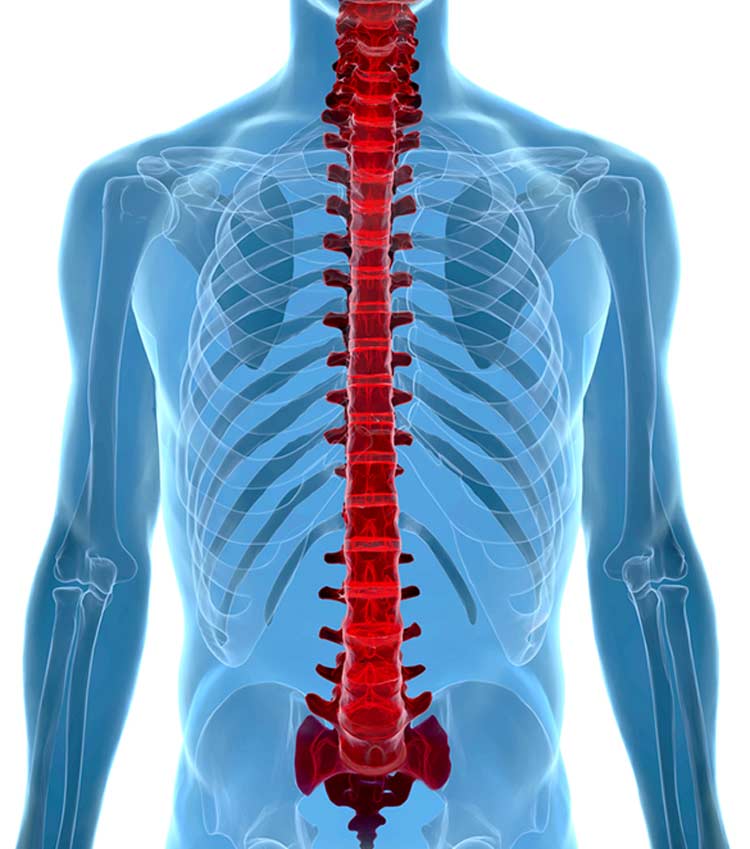
A popular trend in the medical field is outpatient laser spine surgery for neck and back pain–and for good reason. This relatively new approach is considered to be more effective and precise than other methods of spine surgery.
At our center, we use other approaches that are minimally invasive and achieve benefits such as short recovery times, small incisions, and less pain. Our doctors actively integrate the latest state-of-the-art technologies for our patients whenever possible.Spinal surgery may be performed in order to:
- Relieve pain
- Stabilize the spine
- Decrease pressure on a nerve
- Remove a damaged portion of a disc
- Remove bone spurs
- Fuse the spine to promote stability
 Shorter Recovery
Shorter Recovery
With other methods of spine surgery, patients are looking at four to six weeks or longer of recovery time–and that’s for sedentary jobs. With laser spine surgery, patients can be back gradually to part-time work in just one to two weeks (although results may vary).
 The Right Fit
The Right Fit
Every patient is different, and that’s why our doctors work hard to choose the right treatment approach for you. You will be examined and screened prior to any surgery recommendation, and will likely need to try non-surgical relief methods first. If these methods do not work, then outpatient laser spine surgery could be the step you need.
 Small Incision
Small Incision
The incision with laser spine surgery is typically less than one inch in length. A smaller incision contributes to a shorter recovery with less time spent on things like bandage changes. It also reduces your risk of post-surgical infection, which can put your mind at ease after surgery
 An Outpatient Procedure
An Outpatient Procedure
You won’t need to worry about being uncomfortable in a hospital at night, because laser spine surgery is performed on an outpatient basis. This means that you can go home after the procedure and recover where you are most uncomfortable. As long as you have a loved one available to drive you home, and you follow all of your post-surgery directions, your recovery is likely to be smooth.
Many types of spine-related pain can be treated with outpatient laser spine surgery. Lower back pain is one of the most common types of back pain that can sometimes become enough of a distraction to require a doctor’s visit and an eventual referral to a specialist. The muscles, tendons, and ligaments in the lower back often act as shock absorbers during your normal movements. This is also where pressure is often felt as you bend, twist, and sit. Possible sources of low back pain include:
- Bulging or herniated discs
- Spinal stenosis (abnormal narrowing of the spine)
- Spondylolisthesis (lower back disc slips forward over the one below it)
- Lumbar vertebral fractures
Most instances of lower back pain will go away with a little rest, over-the-counter medications, and the application of heat or ice. However, there are times when occasional discomfort turns into chronic pain, defined as pain lasting 3-6 months or more. If conservative treatments aren’t effective and a clear source of pain can be identified with image testing, you may be a candidate for laser spine surgery.
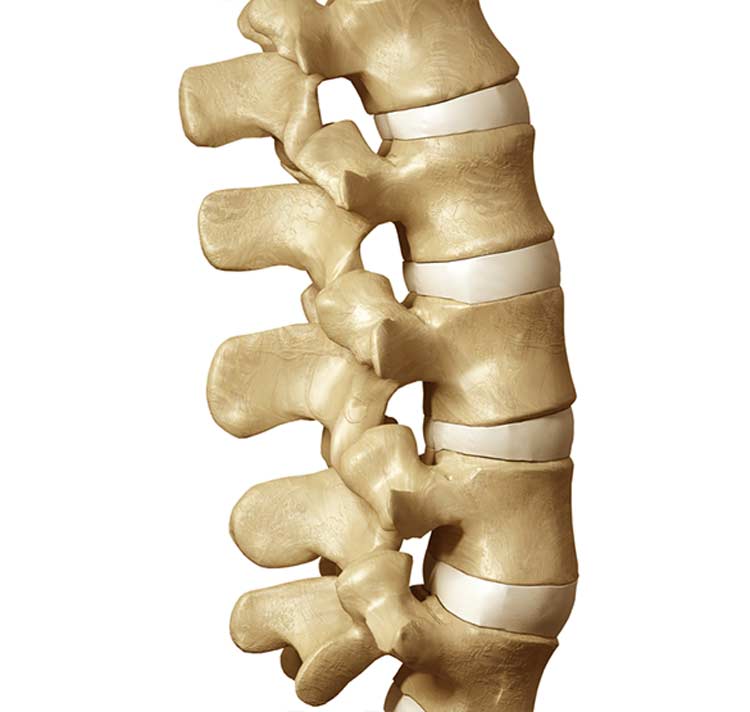
Minimally Invasive Decompression Surgery
There are two main types of laser spine surgery that may provide much-appreciated relief — decompression and stabilization. For most patients with back or neck pain related to a compressed nerve, decompression surgery provides relief. The purpose of decompression is take pressure off of pinched or compressed nerve roots. Disc herniation, spinal stenosis, and bone spurs are among the most common sources of nerve-related back or neck pain.
With a minimally invasive discectomy performed for decompression purposes, only the disc material that’s protruding or pressing on a nerve root is removed. Stability of the spine is not affected. This type of discectomy often benefits patients with disc problems related to degenerative disc disease (age-related disc damage) and sciatica that may be contributing to leg pain and difficulty with mobility.
Nerves near the spine may also be decompressed with a minimally invasive foraminotomy. It’s a procedure done to relieve nerve pressure from foraminal stenosis, the narrowing of a passageway located on both sides of the vertebrae (foraminal canal). If a compressed nerve is affecting the back of the spinal cord, a minimally invasive laminotomy may be more appropriate. During the procedure, part of a small bone (lamina) is removed to free a compressed nerve.
Laser Spine Surgery for Stabilization
The spine sometimes becomes unstable following decompression surgery, usually after a damaged disc has to be fully removed. If this is the case, stabilization surgery is usually necessary to restore the integrity of the spine. Fortunately, there are minimally invasive stabilization surgery options that can be performed as outpatient procedures. With stabilization procedures, the damaged disc that was removed with a discectomy is replaced with an artificial disc. With some procedures, a spacer is inserted to maintain spinal height.
Patients with a diseased or damaged cervical disc that’s causing chronic neck pain and/or radiating arm and shoulder pain may benefit from a minimally invasive cervical disc replacement. An anterior cervical discectomy and fusion (ACDF) is a variation on this procedure that’s performed from the front of the neck with the guidance of a special X-ray. For patients with lower back pain related to damaged disc, a minimally invasive transforaminal lumbar interbody fusion (TLIF) may provide relief while also stabilizing the spine. The procedure involves the insertion of a spacer and bone graft into the disc.
Specific recovery times with laser spine surgery will vary, although recovery from same-day, outpatient procedures is typically shorter than what’s experienced with more invasive operations. Patients also benefit from smaller incisions, fewer surgical risks, and no disruption to nearby muscles. Some procedures only require a small bandage. It’s also common to see patients walking with little or no discomfort shortly after surgery is completed.